  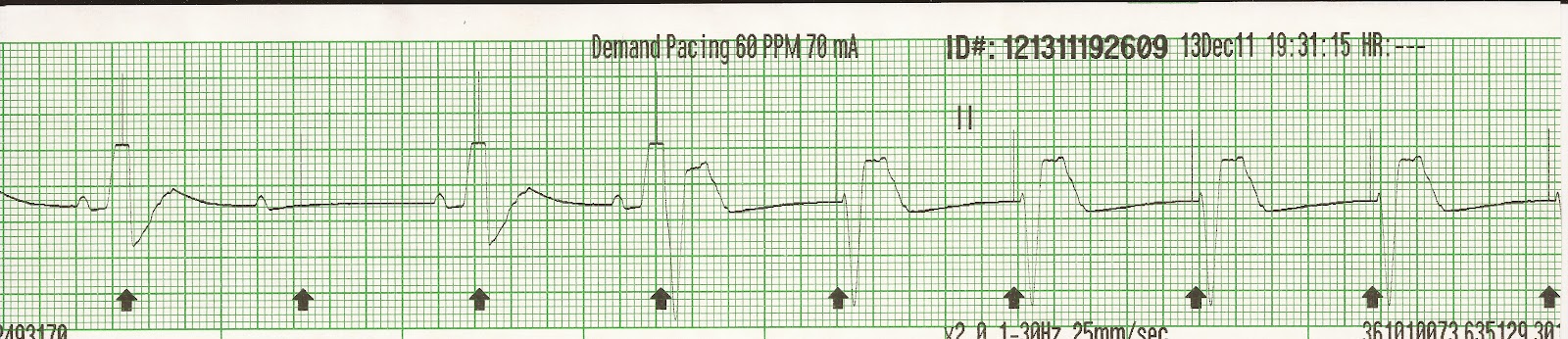
Depending on the pacing site and the atrioventricular (AV) interval programmed, atrial synchronous LVP leads to electrical fusion between the intrinsic excitation of the septum and right ventricle, and the stimulated premature excitation of the left ventricular free wall. The recent European guidelines on cardiac pacing and CRT state that in selected patients with LBBB and conventional indication to CRT, is reasonable to consider LVP alone.Įlectrical fusion between LVP and spontaneous right ventricular activation is considered the key to resynchronisation in sinus rhythm patients treated with single-site LVP. The present availability of devices with separate channels allows the application of LVP while ensuring pacemaker or ICD back-up on the right ventricular lead. Two multi-centre randomized trials have confirmed that there are no substantial differences in response between the two pacing modes. Although indications for LVP must still be clear defined, there is growing evidence suggesting that applying LVP is comparable with the BIVP mode in selected HF patients presenting LBBB. In patients with left ventricular conduction delay and sinus rhythm, LVP alone significantly increases LV systolic function. In comparison with BIVP, single-site LVP is associated with equivalent or better haemodynamic improvement, even during physical exercise. Single-site left ventricular pacing (LVP) confers similar improvements in clinical parameters to BIVP, even in the long term. Most of the available clinical data have been derived from studies involving permanent biventricular pacing (BIVP). In addition, reductions in mortality and hospitalization have recently been demonstrated. These studies have shown statistically significant improvements in quality of life, NYHA functional class ranking, exercise tolerance and left ventricular reverse remodelling. Many observational studies, as well as a series of randomized, controlled trials have demonstrated the safety, efficacy and long-term beneficial effects of CRT. CRT is an adjunctive treatment currently indicated for patients remaining symptomatic in NYHA class III or IV despite optimal medical therapy. Patients with heart failure (HF), low ejection fraction (EF) and left bundle branch block (LBBB) can be treated with cardiac resynchronization therapy (CRT). Using ECG criteria based on the FB may constitute an attractive option for a safe, simple and rapid optimization of resynchronization therapy in patients with HF, SR and LBBB. 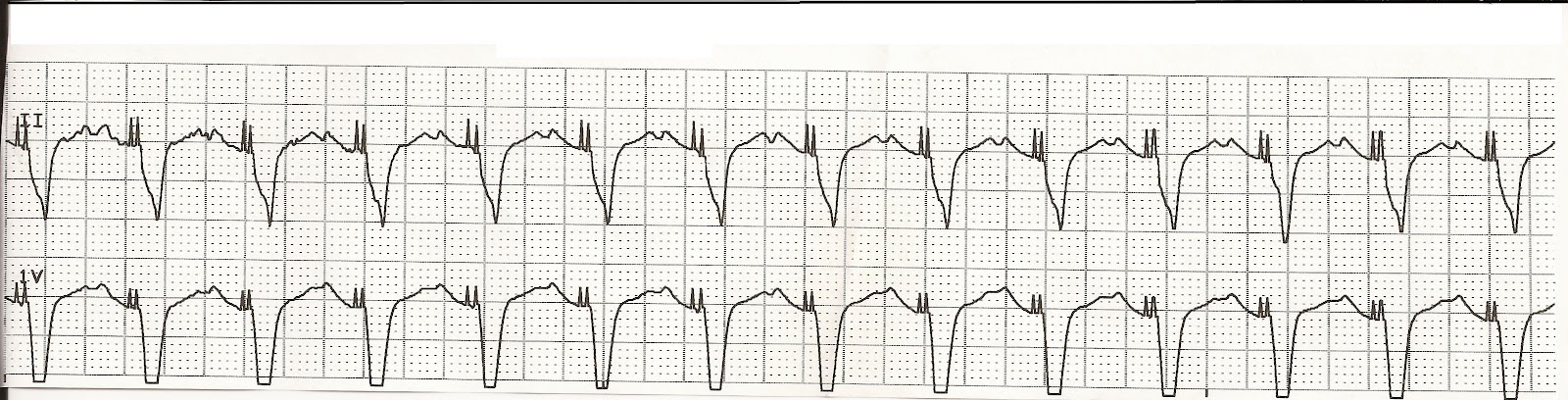
The indications provided by the tested parameters were mostly concordant in that part of the FB corresponding to the shortest AV intervals. The tissue Doppler asynchrony index (Ts-SD-12-ejection) showed a non significant decreasing trend in the FB. Interventricular delay and mitral regurgitation progressively and significantly decreased as AV delay shortened in the FB. Diastolic filling time, ejection fraction and myocardial performance index showed a statistically significant improvement in the FB. 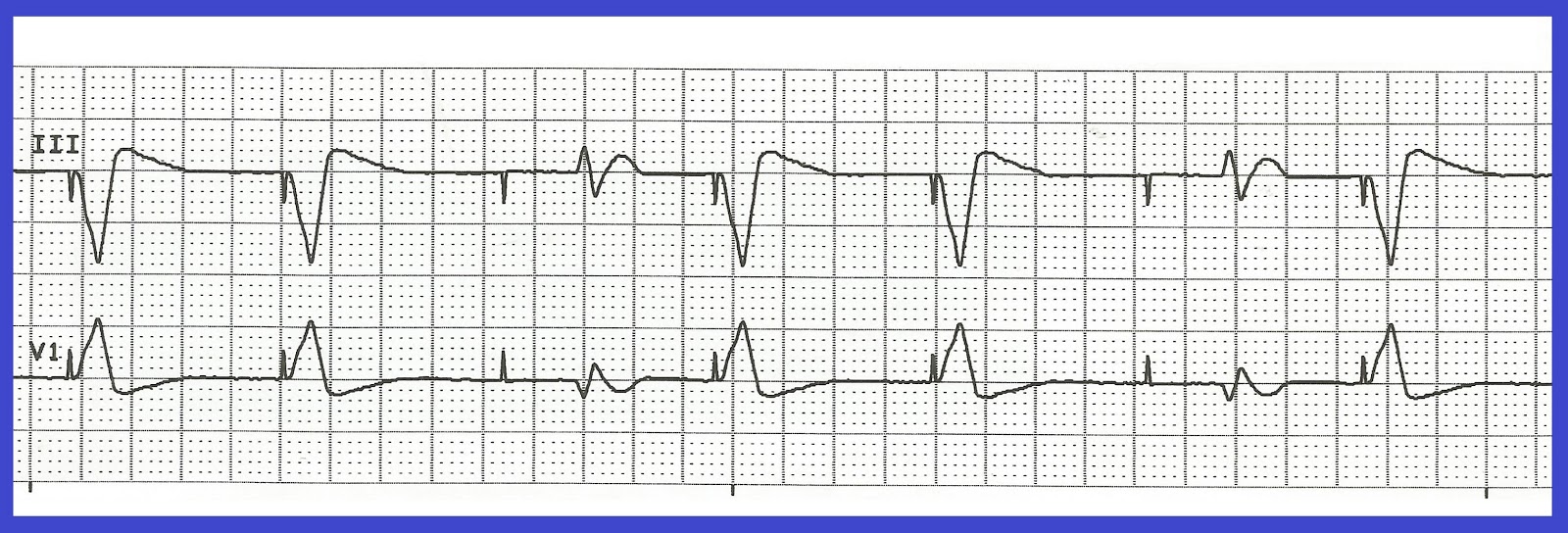
Velocity time integral and ejection time did not improve significantly. Echo-derived parameters were collected in the FB and compared with the basal LBBB condition. We defined the "fusion band" (FB) as the range of AV intervals within which surface ECG showed an intermediate morphology between the native LBBB and the fully paced right bundle branch block patterns. Use of QRS morphology to optimize device programming in patients with heart failure (HF), sinus rhythm (SR), left bundle branch block (LBBB), treated with single-site left ventricular pacing. Electrical fusion between left ventricular pacing and spontaneous right ventricular activation is considered the key to resynchronisation in sinus rhythm patients treated with single-site left ventricular pacing. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
